Are We at the Dawn of “Insulin Socialism”?
The high cost of insulin is one of the great injustices of the US health care system. But now, states like California are looking at directly manufacturing this essential medicine — a potentially massive win for both patients and left-wing politics.
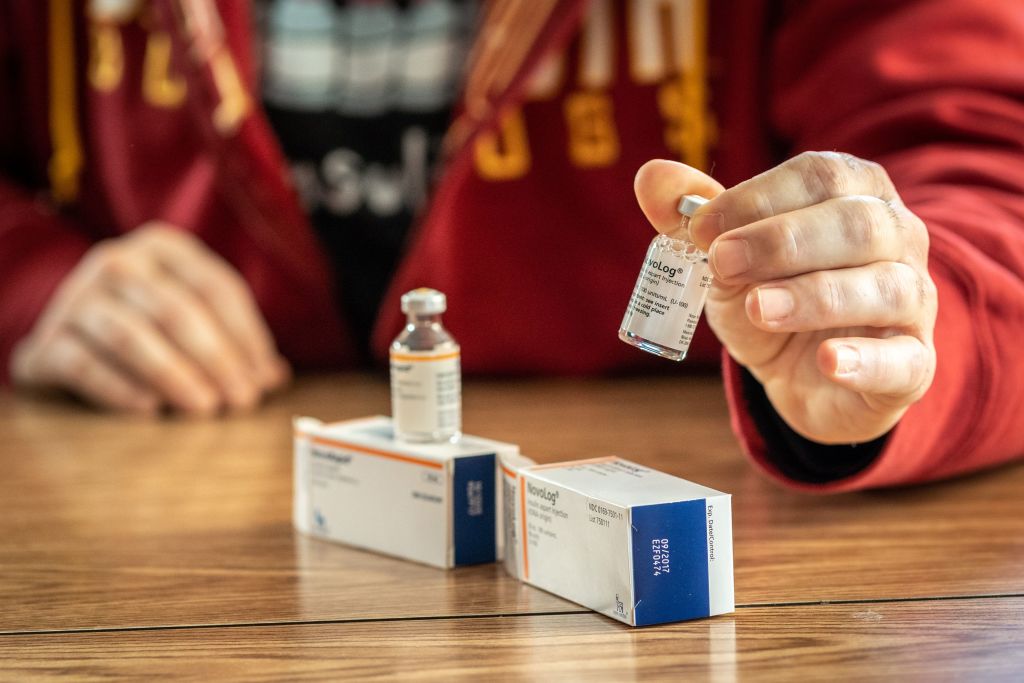
NovoRapid (Canada) and NovoLog (US), insulin drugs sold by Scandinavian company Novo Nordisk. (Kerem Yucel / AFP via Getty Images)
Prior to the invention of the technique to extract insulin from the pancreas of animals in 1921, children with diabetes typically died within a year of the diagnosis. It was a death sentence.
And so the discovery at the University of Toronto by scientist Frederick Banting has to be chalked up as one of the grand medical advances of the twentieth century, almost magical in its transformative power. Physicians at the university described a reversal of fortune like something out of a fairy tale: “Patients . . . were brought into the emergency ward, unconscious in diabetic coma, [and] when injected with insulin they awakened dramatically, snatched from death’s door,” said Bill Bigelow, a young surgeon at the university and witness to early trials of the hormone extract.
Two years later Banting and his colleagues, Charles Best and James Collip, were awarded the US patent for insulin. They sold it to the university for just $1, and Banting refused to put his name on the patent. For a doctor to profit from so essential a medical intervention would be unethical, he believed.
Yet today, the price tag is so high in the United States — more than $300 per vial, or more than $1,000 a month for some if they lack adequate health insurance, up from $21 in 1999 — that one in four Americans with diabetes has to ration their insulin. Diabetes has climbed back up the list of causes of death to seventh place and is the primary driver of liver failure, lower limb amputation, and blindness. It also increases the risk of mortality from heart disease, stroke, cancer, and infections, including from COVID-19. Senator Bernie Sanders has famously taken coaches of patients across the Canadian border to buy the same insulin vials for just $32.
The profiteering from the three firms responsible for all insulin production in the United States — and from other market-driven actors in the American health care system — has become so egregious, and the harm so significant, that the state governments of California, Maine, and Michigan are now looking at manufacturing their own insulin. In Michigan, the man leading the charge for this “insulin socialism” is even a Republican.
This is the tale of how we got to this point, and how such proposals for the “People’s Insulin” could not only solve the insulin crisis, but — if smartly executed — pry open the door to a revival of large-scale, long-term public investment, economic planning, and social democracy in the twenty-first century.
Insulin Is Not Like Other Drugs
The University of Toronto is a university, not a chemical production facility. So after Banting’s groundbreaking discovery, they turned to the noncommercial Connaught Laboratories (originally established in 1914 to mass manufacture diphtheria antitoxin) to produce insulin in Canada. Connaught had a mandate to keep medication accessible, and made the insulin at cost.

For the United States, the University of Toronto turned to Eli Lilly, an American for-profit pharmaceutical chemical production company. In exchange for a one-year distribution monopoly, Eli Lilly would produce the drug. In 1923, it became the best-selling product in the company’s history, generating profits equal to more than half its revenue.
Normally over time, the cost of drugs plummets as the private monopoly of patents runs out and producers of cheaper, generic copies push the price down. That hasn’t happened with insulin, even after almost a century of production.
To understand why, we have to take a short detour to understand what insulin is and how it works.
Insulin is a substance produced in response to food by the oddly named “islets of Langerhans” — clusters of endocrine (hormone-producing) cells in your pancreas. It allows glucose to enter your body’s cells and use it as energy, and tells your body to store any leftover glucose (a sugar) in your liver. In essence, insulin regulates the amount of glucose in your blood.
If your body cannot make insulin properly (type 1 diabetes), or insulin doesn’t work as well as it should or you can’t make enough of it (type 2), your blood sugar is no longer well managed. Not only does your body need glucose for energy (hence the fatigue and extreme hunger that are often signs of the disease), too much of it in the blood can damage blood vessels, organs, and nerves (hence the liver failure, strokes, cardiovascular disease, and amputation).
Where most drugs are typically simple, small molecules made through a relatively straightforward chemical process, insulin is a protein hormone. Proteins are very large, complex, not at all simple molecules, produced by living cells — in the case of insulin, by the beta cells in the islets of Langherans. Remember that insulin was initially produced by extracting it from the pancreases of animals: very early on from dogs, and shortly thereafter from cows and pigs. (Insulin derived from animals is no longer sold in the United States.)
Manufacture of human insulins today involves genetically engineering E. coli bacteria so that they contain the gene for human insulin production, and then deploying these bacteria as insulin factories. Finally, there are also insulin analogues, which are synthetically produced, and are altered to change the rate at which your body takes in insulin. These are very commonly prescribed and can make it easier for people with the condition to plan their meals.
What all these manufacturing processes have in common is that they replicate the complicated production technique of living organisms, often using living organisms or their cells as the “productive facilities.” That is, they are “biologic drugs,” or just “biologics.” (Other biologics include growth hormones, antibodies, and some treatments for arthritis.)
The sheer complexity of insulin production makes it financially unviable for generic drug companies. Thus, instead of generic insulin, we speak of biosimilar insulin — a biosimilar biologic drug, or just “a biosimilar,” is a biologic drug that is extremely similar but not identical to the original. Generic drugs are identical copies of the original but biosimilars are not because the latter’s structure (and that of the original biologic drug that the biosimilar is imitating) depends on the manufacturing process much more than the former’s does.
While the overall method of manufacturing insulin is public information, the specific manufacturing process is a trade secret, a form of intellectual property that does not have an expiration date.
As a result, a biosimilar company must spend a considerable chunk of money to independently reinvent this manufacturing process. The estimated investment for a biosimilar is $100-250 million over seven to eight years, compared to just $1-4 million over a single year for small-molecule generic drugs.
So here’s the bottom line: while biosimilars are a bit cheaper than the original biologic, we do not see price declines comparable to a generic drug company copying the formula for, say, aspirin. This biological nature of the drug and the fact that the manufacturing process enjoys trade secret protection explains why there is not much competition in insulin production (or for that matter, within the production of other biologics). Most of the global producers of biosimilar insulins are companies that already manufacture insulin — because they can lean on their existing knowledge and technology and don’t have to reinvent the wheel like true competitors would.
In addition, with ordinary small-molecule drugs, pharmaceutical companies regularly change the molecules in their products ever so slightly, improving them very modestly, and then re-patent them to try to keep ahead of the generic competitors. This practice of “evergreening” is made that much worse for insulin products and their potential biosimilar competitors by the complexity of biologic production.
All of this explains why the United States’ insulin problem is not just an American phenomenon. Europe has not had much success trying to entice firms to produce biosimilars either.

But the debacle doesn’t stop there. Compounding this biochemical, structural, and manufacturing challenge, most of the pens and other devices used to deliver insulin — devices that are tied to a particular type and brand of insulin — carry their own patents. A potential biosimilar developer therefore also must develop their own delivery devices, yet another barrier to market entry.
Finally, while biosimilars have no expected, meaningful differences in effectiveness or safety, because they are similar not identical, they are subject to additional studies before receiving regulatory authorization. Unlike generics, biosimilars are not automatically substitutable for the original. They have to show they produce the same clinical result and do not pose any greater risk. These extra studies and authorization steps further inflate the cost. Consequently, even laudable intellectual property reform — such as allowing limited disclosure of the manufacturing process and standardization of devices — would only modestly mitigate the cost spiral problem.
One way to attack the more fundamental issue — the biological nature of the drug — would be to ease approval of interchangeability of the original biologic drug and its biosimilars. This has happened in other jurisdictions, and in 2020, the US Food and Drug Administration (FDA) released some new guidance with this aim in mind while also approving its first biosimilar, Semglee, a long-acting insulin analogue produced by pharma companies Biocon and Viatris that mimics Sanofi’s Lantus insulin product. Then in July 2021, the FDA awarded its first-ever interchangeable designation to Semglee.
Still, biosimilars tend to yield price reductions of about 15 percent, compared to 50-80 percent for generics. Sanofi’s Lantus runs at about $280 per vial, or $425 for a box of five pens, while the initial wholesale list price of unbranded Semglee product is just $99 per vial, or $148 for the five pens — a marked drop, but still much higher than in Canada. Viatris priced Semglee at the same sticker tag as Lantus pens in 2007, and Lantus insulin vials in 2010. Their target is those without insurance or with high deductibles who need to pay for their insulin in cash.
The Manchin Family Maneuver
Viatris’s action on insulin is a genuine improvement, enabled by the FDA’s smart intervention to ameliorate a pathology of market behavior.
But who is Viatris? Why are they getting in the game? Funny you should ask.
Viatris is the new name for the firm Mylan, whom you may remember as the producers of the EpiPen — the epinephrine auto-injectors that many food allergy sufferers depend on to treat incidents of anaphylactic shock. Mylan steadily jacked up the price of a two-pack of EpiPens from $124 in 2009 to $609 in 2016, prompting a public outcry that forced the firm to issue a generic alternative with a lower (but still scandalous) $300 price ticket.

Mylan, which controlled 96 percent of the US market for epinephrine auto-injectors, was able to engage in these shenanigans by colluding with Pfizer, the owner of EpiPen’s competitor, Adrenaclick. Pfizer withdrew Adrenaclick from the market, delivering a monopoly to Mylan, in return for a cut of the price-gouging proceeds, which would allow Pfizer to earn more than it would by producing a cheaper competitor. (Interestingly, over the course of this price-gouging episode, Mylan was among the largest donors to the campaign of Democratic senator Joe Manchin, who is also the father of Mylan’s CEO, Heather Bresch. As the Intercept revealed last year, her mother, Gayle Manchin, then head of the National Association of State Boards of Education, encouraged states to force schools to stock her daughter’s lifesaving and, very expensive, monopoly commodity.)
Mylan ultimately dropped its tarnished name. Producing Semglee is another means to launder its terrible brand. And Mylan/Viatris is able to do so while not really losing out on the insulin bonanza: Semglee also comes in a branded version, targeting insurers and pharmacy benefit managers (more on these middlemen and the unique bit of devilry they get up to in the United States shortly) at about $270 per vial, or roughly $400 for five pens. This still ends up costing the US system far more than other nations spend.
And even the $99 unbranded vial of Semglee — sufficient for a few days to weeks for some — is a rip-off. A 2018 analysis of the costs of inputs and manufacturing processes of insulin production appearing in the British Medical Journal in 2018 showed that treatment with insulin analogues such as Lantus or Semglee could cost $133 or less per year.
And all these options — speeding up biosimilar approval, easing interchangeability, trade secret disclosure, standardization of devices — would instantly provoke stiff opposition from the big three insulin producers: Eli Lilly, Sanofi, and Denmark’s Novo Nordisk, which control the entire US insulin market and 90 percent of the global market.
Even with aggressive antitrust enforcement, the barriers to entry due to the biologic nature of the drug are still so considerable and the existing market control so thorough, that other firms are likely to be dissuaded from even trying. Were a new, private biosimilar competitor to attempt to establish themselves in the United States, or anywhere else, the Big Three could temporarily lower their prices and undercut the upstart. Merck and Samsung Bioepis abandoned their entrance into the US market for just this reason, and Novo Nordisk has likewise priced out Indian competitors. As Yale health law scholar Ryan Knox wrote in a 2021 overview of the problem: “The hold of the Big Three on the global insulin market makes it questionable whether it is ‘financially viable’ for new biosimilar manufacturers to enter the market . . . [e]ven though insulin could be sold at much lower prices and still yield profits.”
Walmart to the Rescue?
In July 2021, Walmart introduced its own brand of the rapid-acting insulin analogue, NovoLog, as part of its ReliOn suite of health products. The price tag: $73 per vial.
“A typical patient using two vials of rapid-acting insulin per month will spend $1,749 per year for Walmart’s ReliOn Novolog,” said Hilary Koch, policy manager of the diabetes advocacy group T1Interational (which, unlike many patient advocacy groups, refuses funding from Big Pharma). “While much less than the $6,945 full list price, this is still a very high price for an essential drug.”
For comparison, the ticket price is $6-13 per vial across the rest of the OECD (Organisation for Economic Co-operation and Development, the club of developed nations), and the cost to manufacture and bring to market rapid-acting analogue insulin is $6-7 per vial.
In addition, the ReliOn insulin wears Walmart’s private label, but is manufactured for the store by Novo Nordisk, one of the insulin Big Three. Has Novo Nordisk decided out of the good of its heart to give up on the big bucks?
Unlikely. As seen with the Mylan/Viatris play, a common tactic of pharma firms facing public scrutiny is to partition off a very low-income segment of the market, either through means-tested rebates or a cheaper version marketed at that demographic. Novo Nordisk may be hoping that by swallowing these losses, politicians and the media will call off the dogs and allow them to keep rolling in dough in more lucrative segments of the market.
But even here, it remains to be seen how Sanofi and Eli Lilly will react to the Novo Nordisk–Walmart gambit, or whether, as with a play by another of the Big Pharma beasts, they just temporarily undercut them to force them to withdraw their product.
T1International isn’t taking any chances: it has called for the introduction of a federal price cap instead of depending on the suspicious generosity of Walmart and Novo Nordisk.
White-Hatted Capitalist Charity
A more interesting recent play has come from Civica Rx, a consortium of philanthropists, health care providers, and insurers. While comprising both nonprofit and for-profit entities (including Blue Cross Blue Shield and Kaiser Permanente), the Utah-based consortium as a whole is not for profit, and already produces some sixty different generic drugs. In March 2022, Civica announced they would also manufacture and distribute three different insulin biosimilars without regard for profit, all for no more than $30 per vial or $55 for a box of five pens. As mentioned, biosimilars tend to take many years before commercial availability, and Civica Rx has acknowledged the hurdles in front of them while setting a tentative release date of 2024.
Civica is certainly to be applauded, but the rationale behind the operation, as the group’s website admits, is to deliver millions of dollars in savings to the consortium’s hospital systems, both not-for-profit and private. The aim is to “create market stability” and “guarantee volumes” for their partners’ needs. The soaring cost of insulins (and other drugs) is not just bad for patients; it’s bad for hospitals and insurers too. Civica’s charitable endeavor is thus also just a sensible business decision. And if patients are better off as a result of one set of capitalists getting frustrated with another set of capitalists, does it really matter that the former are only doing it for the sake of the bottom line?
Not really, no. But this dynamic also means that if at any point their endeavor ceases to be a sensible business decision — if the Big Three use their market power and exploit the unique characteristics of insulin production to put on the squeeze, and it no longer is in the interest of the “white-hatted” capitalists in the Civica consortium — then they will likely pull out.
That may explain why California governor Gavin Newsom — who had earlier considered partnering with Civica Rx on generics and insulin biosimilars — and Maine and Michigan decided to push out on their own. And there’s certainly no harm in both a public option and a charitable option working separately (or joining forces) to push down prices.
The Dastardly Middlemen
Beyond the unique characteristics of the biological production of insulin, there is also some extra special American sauce in the mix that makes the situation particularly egregious compared to anywhere else: the pharmacy management companies (PBMs or pharmacy benefit managers).
PBMs are private companies in the US health care ecosystem that act as intermediaries between drug manufacturers, insurers, and pharmacies. Three dominate the sector: CVS Caremark, a subsidiary of CVS drugstores; Express Scripts; and OptumRx. Insurers contract PBMs to handle negotiations over drug prices with the producers, as well as handle insurance claims and the distribution of drugs. The original point of PBMs was to take advantage of the aggregate buying power of their client insurance firms to bargain down the cost of drugs.
It hasn’t worked out as planned.
Drug manufacturers lose out on big chunks of the colossal US pharmaceutical market if their products do not end up on “formularies” — lists of the drugs that will be covered by a health insurance plan. Who gets to decide which drugs will appear on the formularies? You guessed it: the PBMs.
In order to keep in the PBM gatekeepers’ good graces, drug manufacturers pay the PBMs kickbacks that they call “manufacturers’ rebates.” The rebates, which are calculated as a percentage of a drug’s “list price” (aka the sticker price), ensure that the PBMs deliver preferential placement on the formularies to a manufacturer’s drugs: “You got a nice drug there, Larry. It’d be a shame if, you know, it fell off the formulary.”
To cover the cost of this bribe — sorry, rebate! — the manufacturers simply hike up the sticker price. This happens with all drugs, but as a US Senate report found, the insulin situation is just that much worse. The PBMs make an expensive thing even more expensive. According to the president of Eli Lilly, the cost of the rebates makes up 75 percent of the list price of the company’s insulin products.
We often lament the villainy of Big Pharma, but we might also want to offer a little consideration for the perfidy of the shadowy middlemen, the PBMs, who operate out of the view of regulators, consumers, and the media, and bring in more than $200 billion annually to manage prescription services for insurers. PBMs are one of the reasons that while the United States represents only 15 percent of the global insulin market, it is responsible for almost half of all revenues from insulin.
PBMs are so egregious, in fact, that both Democrats and Republicans are now looking at cracking down on them. In May, Republican senator Charles Grassley joined with Democratic senator Maria Cantwell to introduce legislation empowering the Federal Trade Commission and state attorneys to go after “unfair and deceptive” PBM practices that ramp up drug prices. Other Republican senators, including New Hampshire’s Jeanne Shaheen and Maine’s Susan Collins, are backing legislation capping PBM insulin rebates.

But don’t somehow think drug makers’ hands are clean. In May 2017, a lawsuit filed in a Los Angeles federal court alleged that one of the insulin Big Three, Novo Nordisk, colluded with the PBM OptumRx in an “illegal pricing scheme” to inflate the price of Victoza, a diabetes drug (not an insulin, but a complementary medication for type 2 diabetes that helps control blood glucose).
And even if the PBM crackdown is successful, it won’t solve the deeper problem that stems from insulin’s special characteristics.
The Canadian Option
Insulin’s unique characteristics have led some clinicians, chemists, and public health officials to call the drug a natural monopoly. “Unlike small molecules that are granted artificial monopolies, biologics are best described as natural monopolies,” a quartet of clinical specialists wrote in Health Affairs last year. “They are protected by barriers to entry stemming from the scientific uncertainty that arises from their structural complexity; these barriers are expensive, time-consuming and risky to breach.”
As a natural monopoly, they argue, insulin requires some form of price regulation to prevent producers from charging whatever they like. This could take a number of forms. The Centers for Medicare and Medicaid services could refuse to pay the higher price for the originator drugs and only buy biosimilars. The secretary of Health and Human Services could negotiate drug prices on behalf of all Americans. There could be limits on pricing that permit cost of production plus some top up, or prices that deliver a restricted return on investment or some other specified margin. In other words, price controls.
These are all creative ideas. And aren’t price controls how Canada keeps its insulin costs so much lower than the US anyway? That’s certainly part of the story.
In 1987, Canada’s parliament established the Patented Medicine Prices Review Board, a quasi-judicial body that offered pharmaceutical companies a quid pro quo: we give you increased patent protection, and you agree to direct price regulation of your drugs. The price board sets a maximum price after considering the average price of a basket of eleven comparable countries in Europe as well as Japan and Australia (the United States used to be a comparator too, but was recently dropped due to its outlier prices skewing the average).
On top of this, the Canadian federal government and the provinces use their joint purchasing power to negotiate the price of a drug even lower. The ultimate aim — at least on paper — is the creation of a national pharmacare program that wraps pharmaceuticals into the Canadian single-payer health care system (although there are big fights ahead for that battle to be won).
Pharmaceutical companies regularly whine that price regulation Canadian-style would inhibit innovation, but a 2021 US House report found that Novo Nordisk, for example, spent more in stock buybacks and dividend payments than on research and development in each of the last five years.
So could the price control approach work in the United States?
The California Option
Some states have capped out-of-pocket insulin costs for those with insurance. Nevada mandated insulin pricing transparency in 2017, and two years later Colorado became the first state to institute an actual price cap on insulin. In April, House Democrats managed to pass the Affordable Insulin Now Act with the help of twelve Republicans. The act would cap the cost of insulin at $35 a month — again, for those with insurance, and could allow Medicare to directly negotiate the price of insulin with drug makers, akin to the Canadian system. (The bill, now wrapped into the omnibus Inflation Reduction Act, still has to pass the Senate.)
No one, however, is capping the cost of insulin for the uninsured.
Thus, due to the vagaries of the US political system, state-level “insulin socialism” — the government directly manufacturing the drug — may ironically be easier to achieve than the ostensibly more modest and less interventionist approach of cross-the-board price regulation. Regardless, it certainly would complement price caps, attacking the insulin challenge from another flank. It should also drive costs lower still, as well as expand supply and avoid displacement of the problem to the rest of the world as the Big Three attempt to recoup any losses in the United States by squeezing other jurisdictions.
And ultimately price caps, as necessary as they may be, are stopgap measures. Canada may have price regulation, but prices are climbing there too. A 2016 analysis by the country’s price review board found that from 2010 to 2015 the average cost of insulin jumped over 50 percent, far above inflation. The price increases of all other drugs in Canada over the same period sat in the low single digits at most, due to the impact of competition from generics. The board concluded that the insulin price spike was driven by evergreening — in this case, the greater use of newer, more expensive long-acting insulins by the Big Three.
The underlying problem of control of production by an oligopoly remains unsolved.
This may be another reason why California is opting for a more aggressive approach. California and Canada have roughly the same population (39 and 38 million, respectively). If Canada’s aggregate purchasing power is beginning to struggle to keep prices low, California is unlikely to fare any better.
Creating public drug companies is not pie-in-the-sky fantasizing. Around the world, from Sweden and the UK to India and Massachusetts, there are pharmaceutical companies that are owned by the public and both produce drugs that private firms find insufficiently profitable and act as a public competitor that drives down the cost of drugs made by private producers. These firms can also operate elsewhere in the pharmaceutical supply chain, from manufacture of chemical or biological inputs to distribution and retail.
By operating outside market imperatives such as profit maximization and rent-seeking, public drug enterprises are free to prioritize public health, scientific advancement, economic development, and researching potentially non-lucrative drugs and other therapeutics (including for rare diseases), combatting shortages, creating surge capacity in emergencies, and smoothing out price volatility at other times.
In recent years, momentum for an insulin public option has been picking up.
In 2018, Senator Elizabeth Warren came out in favor of the federal government creating its own insulin biosimilar production facility. This year, Michigan state senator Curt VanderWall, a Republican, introduced a scheme for the state government to manufacture its own insulin and sell it to Michiganders at cost, hopefully at around $50 per vial. VanderWall said he believes the plan would allow the state to circumvent the PBMs.
Joining Michigan’s efforts, in May, Maine passed legislation creating a commission to investigate whether the state could also produce its own insulin in tandem with the University of Maine. With its smaller size, the state may not have the resources or a big enough market, so the government says it’s open to exploring partnerships with the private sector or other states, and is petitioning the federal government to take action.
And last month, in the most concrete “People’s Insulin” action taken, the California state budget — recently signed by Governor Gavin Newsom — allocated $100 million for the state government to contract and manufacture its own insulin via a public enterprise called CalRx and sell at “close to cost,” available to all. The details still need to be hammered out, but it looks like $50 million of the sum will go to developing low-cost interchangeable biosimilar insulins and the other $50 million toward building a California-based insulin manufacturing facility.
At $100 million, this is on the lower end of the aforementioned average costs for biosimilar production, but still within the range. So what are the chances of success?
“Other States Might Go: ‘Oh Wait, I Could Do That Too’”
Paul Williams, the head of the Center for Public Enterprise, a US think tank that promotes public option goods and services along the lines of what California is planning, says the state is picking a fight with some real bruisers.
“The Big Three have gone toe-to-toe with folks like Merck, with Indian generic manufacturers, who have much more experience with this sort of thing than Sacramento — and won,” he told Jacobin. Merck is the seventh-largest pharmaceutical company in the world, and one of its major products, Januvia, is one of the biggest selling diabetes drugs worldwide, albeit not an insulin.
“They’ve got game. If they can price out a hulking beast like Merck, they’re probably confident they can do the same with the state of California.”
But Williams believes the concept is sound and that California, as the most populous state in the union, has a better shot than maybe anyone else. Even more important, other potential competitors like Merck and Indian producers of generics that were squeezed out are also for-profit companies. A state can weather the storms of losses in a way that for-profits cannot.
If CalRx’s insulin gambit succeeds, it would force other suppliers to permanently drop their prices to compete.
“The idea of a public option got a bad rap from Pete Buttigieg when he was talking about it as an alternative to Medicare for All,” adds Williams. “But that was in the context of trying to defeat a far better alternative that already demonstrably works in many other countries.”
So imagine: a state-owned insulin company acts as a public competitor aiming to euthanize the rentier in oligopolistic markets. It succeeds in sharply reducing insulin pricing and breaking the back of the insulin oligopoly — securing a massive, high-profile victory that demonstrates the public sector’s efficacy after decades of neoliberal demonization of economic planning and public ownership.
“Other states might go: ‘Oh wait, I could do that too? And for other drugs?” says Williams. “CalRx can operate as a demonstration project, showing the feasibility of public enterprises, which can then begin to expand to not just other drugs, but also other sectors, de-risking innovation, smoothing out price volatility, overcoming supply chain shortages — in other words, shaping markets rather than just letting them rip.”
Of course, lots of questions remain. Will CalRx’s insulin be restricted to the Californian market, and therefore only drive these price effects in the Golden State? Could the Golden State join up with the likes of Michigan and Maine to spread lower insulin prices nation- (or even world-) wide?
What responsibility does California have to the rest of the country? To the rest of the world’s insulin patients? If California were to sell its insulin outside its borders for profit to help fund the nonprofit program in the state, it would begin to have an interest in high prices elsewhere — no different from the Big Three.
This is effectively what happened with Novo Nordisk. It is the profit-making arm of the wealthiest charitable foundation in the world, the Novo Nordisk Foundation, which focuses on medical research. Novo Nordisk exists to bankroll the foundation, which hands out hundreds of millions each year to scientists, clinicians, and various humanitarian projects. And yet Novo Nordisk has also, for example, been the object of a 2019 class action lawsuit alleging that it, together with Eli Lilly and Sanofi, engaged in an “arms race” to boost insulin list prices.
These latter issues are soluble, so long as California commits to maintaining a nonprofit ethic throughout its insulin efforts. It is the market that is the ultimate cause of the problem, rather than “corporate-ness,” size, or corruption.
Insulin Socialism?
The vision above of a stepwise approach to building back the role of public enterprise may strike some socialists as overly wonkish or insufficiently comprehensive in its demands. Some may dismiss it as mere “social democracy,” rather than socialism.
Frankly, so what? All the grand projects of democratic socialism that prompt such admiration in the United States and elsewhere — Canada and Britain’s health care systems, Austria’s public housing, the panoply of Scandinavia’s social programs and public ownership — began with smaller, sectoral, or regional demonstrations that later made the much more comprehensive versions feasible. The province of Saskatchewan delivered single-payer health insurance first, years before it was adopted at the national level. The UK’s National Health Service modeled itself on worker cooperative societies, but on a nationwide scale. People saw how these socialized and cooperative modes of enterprise had already worked very well, far better than their private counterparts, and now trusted that they could work on a larger scale.
Nor does this stepwise approach exclude the necessity of social struggle in the workplace, in the streets, and in neighborhoods to win concessions from elites, or of the need to take legal action against cartels. On the contrary: they all work together. Street-level fury — such as the protests outside the offices of Sanofi and Eli Lilly of parents who lost their children due to insulin rationing, holding their children’s ashes as they did so — generates the political will needed to pass regulations or set up public enterprises.
History also shows that progressive measures can come from unlikely sources. In the decades after World War II, it wasn’t just European social democrats, but also center-right parties that introduced welfare state measures: the workers movement, through its trade unions and parties, sharply shifted the political terrain to the left. Elites were afraid that if they did not give up some of their power and wealth to deliver social reforms, they would be rendered irrelevant.
We’re not at that point today. The US labor movement is still weak, and many baseless, evidence-free tenets of neoliberalism still reign in the Democratic Party. But the shifting political winds since the 2008 financial crash have opened up new possibilities for policies that at least concede some ground to classical socialist demands for economic planning. Indeed, this helps explain why insulin socialism is being touted by moderate Democrats and even Republicans: it’s enormously popular amid the widespread anger at insulin injustice.
Socialists would be wise to take up this policy and mold it to our own ends — a “people’s insulin” rather than a “California-only insulin.” That will mean pressuring Democrats like Newsom and Republicans like VanderWall: if CalRx is tempted by for-profit sale outside California or beyond the United States, the Left must explain why doing so would pit one set of insulin users against another, and to organize opposition.
The Left must also push to extend the public enterprise principles behind state manufacturing of insulin to state manufacturing of other drugs — alongside allied government interventions such as price regulation, conscious use of procurement to shape markets, and intellectual property reform — and then to other sectors. Insulin is far from the only good or service suffering from oligopoly, supply constraints, and antisocial price effects. Success with these cases would give us further social license to push for still-greater levels of intervention, such as nationalization and industrial policy.
Over the long term, the ambition of this stepwise strategy is even grander. The prize is a suite of pro-worker policies prioritizing public welfare and prosperity over the market across the board rather than just as a one-time fix correcting the flaws of a particular market failure.
Ultimately, what is exciting about California’s public insulin project is that it is another — but this time more ambitious — example of the new mood that breaks with the previous four decades of neoliberal “common sense” telling us markets know best. And CalRx is not just venting fury at a rigged system: it’s a well thought out, credible step by America’s largest state to tackle the profound injustices of the country’s most expensive chronic condition.
At a time when disappointments abound, this is a potentially major development in the practical process of unrigging that system.