Medical Debt Collection Is a Vicious Multibillion-Dollar Industry in the US
Medical debt has ballooned in the US in recent decades. Hospitals and collection agencies are making a killing on it, eroding trust in the health care system and leading countless patients into financial ruin in the process.
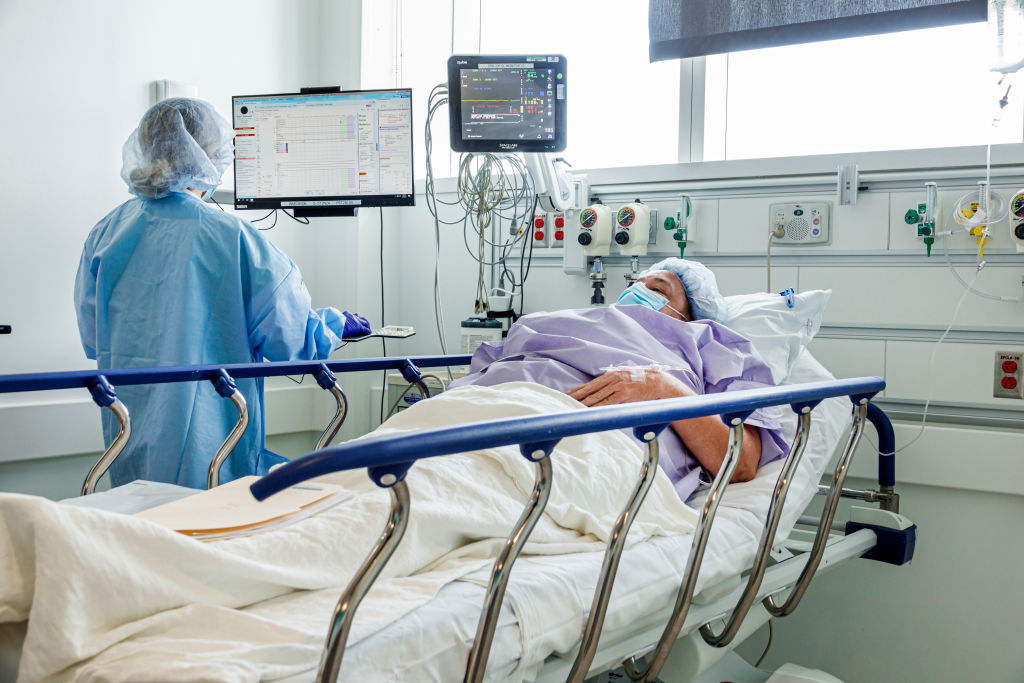
A patient and nurse in Mount Sinai Medical Center, Miami Beach, Florida. (Jeffrey Greenberg / Universal Images Group via Getty Images)
- Interview by
- Sara Van Horn
- Cal Turner
“Receivables Management Association” may not mean much to the average American. But this professional association — which changed its name from the more straightforward “Debt Buyers’ Association” in 2017, following media scrutiny of its practices — represents a burgeoning industry in the United States: medical debt collection.
As of March 2022, forty-three million Americans had medical debt on their credit reports. Much scholarship and reporting has shown how medical debt has ballooned in the United States over the past several decades, but the mechanisms by which debt is being pursued every day remain less visible.
In Your Money or Your Life: Debt Collection in American Medicine, emergency physician and historian Luke Messac traces medical debt collection from its beginnings to its current incarnation as a multibillion-dollar industry. Messac describes how medical debt has eroded trust in American health care and led countless patients into financial ruin. He draws from his experience as a doctor to argue that medical debt collection puts the foundational relationship between patient and provider, and the physical and financial health of patients across the United States, in grave danger.
Cal Turner and Sara Van Horn spoke with Messac for Jacobin about the brutal tactics — like garnishing wages, foreclosing on homes, and even arresting patients — that hospitals and collection agencies use to collect unpaid debts, the ripple effects of debt collection on patient health and trust in the medical system, and the efforts underway to eliminate the practice.
Sara Van Horn
Could you give a brief history of medical debt in the United States? How and when did it become so widespread?
Luke Messac
Medical debt itself isn’t new. There’s been medical debt in this country since doctors and midwives started treating patients.
During the nineteenth century, private-practice physicians were responsible for collecting their own patients’ payments. It was an intensely personal relationship, and there was an idea that you couldn’t risk the relationship by collecting debt too aggressively. That’s not to say it didn’t happen, but there was some modicum of professional responsibility for maintaining the relationship even in the face of unpaid debts.
Hospitals, for their part, developed out of almshouses, and for centuries the expectation was that they were the site of care for the poor. But by the early part of the twentieth century, hospitals started to abandon their former identity as bastions of charity.
Private nonprofit hospitals now had new technologies and sought-after procedures and were places where most patients were expected to pay for their care. Hospitals had their own billing departments. They could be aggressive, but oftentimes they would let that debt sit on books for years or decades.
Debt was a problem in midcentury America. It was the subject of books and congressional hearings and was one of the major concerns that drove advocates for universal health care. Though that goal wasn’t reached, the passage of Medicare and Medicaid and community health centers were all responses to the growing problem of people unable to afford necessary medical care.
The era of aggressive medical debt collection really began in the 1980s and 1990s, when Medicare and Medicaid reimbursements started to plateau. This was the era of neoliberalism, the era of Ronald Reagan saying that we shouldn’t be spending so much on the unworthy poor.
In response, more hospitals hired third-party debt collectors. Hospital financial executives were saying, “We’re not going to wait anymore for that money.” Whatever could be done to collect debt became the norm: putting liens on patients’ homes, garnishing their wages, taking them to court, reporting their debt to credit bureaus, refusing care for nonemergent services — even seeking their arrest if they didn’t show up for court hearings.
Cal Turner
What actors were involved in deploying these new tactics? What were their motivations?
Luke Messac
The story of debt collection in the United States is the story of who foots the bill when the patient can’t afford to pay. For a time, that responsibility was on hospitals through the provision of charity care. Later, the federal government took on that role with Medicare and Medicaid, but eventually those reimbursements started to decline relative to costs.
During the 1980s, private insurance companies paid more than the cost of care for the individuals they covered, which helped make up some of the shortfall. But when all these actors decided it was no longer their responsibility, who was left? Eventually it all fell to the patients. Once it did, hospitals turned toward collectors.
Debt collection agencies can be small, fly-by-night operations, or they can be large, publicly traded corporations with thousands and thousands of collectors at call centers around the world. Often, those companies receive a contingency fee on whatever they collect from patients, and whatever they can’t collect reverts back to the hospital after an agreed-on period. That’s the most common arrangement.
Another common arrangement is hospitals selling patient debt to collection agencies outright. A hospital will put that debt up for sale, and that debt is bought by a debt buyer — which could be the same collection agency that does the work on a contingency basis, or it could be an investor who simply buys and sells the debt. These groups often work that debt very hard because they have no connection to the patients. These are just numbers on a sheet of paper, and the more they collect, the more money they get. The arrangement becomes strictly financial and therefore subject to more aggressive collection.
Sara Van Horn
What are the possible destinies of a medical debt once it’s incurred?
Luke Messac
There are many ways that a hospital can handle medical debt. I focus on hospitals, and specifically nonprofit hospitals, not only because that’s where a lot of the medical debt originates but also because nonprofit hospitals owe their tax exemption to the community benefits they provide. So one would expect that a lot of these debts might be written off as charity care.
That is one possible destiny of that debt. Unfortunately, it’s not a common-enough destiny. If a hospital decides not to provide a patient with charity care — because the patient didn’t apply for it, or because they were denied it, or because the hospital didn’t let that patient apply for charity care by not telling them they were eligible — the hospital can choose to pursue the patient’s debt in a number of ways.
One way is to handle it internally in a hospital’s own billing and collections departments, which was the common way of handling debt for many decades. Hospitals can send letters, make phone calls, and sometimes visit homes. If the bill is still not collected, then they have a choice: they can decline to pursue the matter any further, or they can turn to other measures. If they take the latter course, they can pursue it using legal avenues, and at this point they might also assign or sell the debt to collection agencies.
The legal avenue opens up a panoply of problems for the patient. When a hospital files a lawsuit in small claims court, oftentimes the patient won’t show up for court and they’ll lose by default. When they do, the hospital now has several ways to collect that debt, including garnishing the patient’s wages or placing a lien on a patient’s property. It can foreclose on a patient’s home. The more aggressive the hospital chooses to be, the more peril that patient is in.
Cal Turner
How does this affect patients’ lives and their relationship to medical care?
Luke Messac
In general terms, this is disastrous for patients. Their financial health is ruined, and their physical health can be ruined. We know that patients forgo care for fear of debt, and that even small increases in out-of-pocket payment requirements lead patients to skip medicine, skip doctors’ visits, or delay coming into the emergency department in an emergency.
The story that sits with me most is Quinton White, who was a seventy-seven-year-old former dry-cleaning employee who was sued by Yale New Haven Hospital for the debt of his wife. For twenty years, he was paying her debt back through payment plans while being charged 10 percent interest. By the 2000s, he owed $40,000, even though he had already paid $16,000, close to the original amount he had owed.
Over those two decades, the hospital had placed a lien on his home and seized his bank account. Mr White’s wife had died of cancer years before, but he was still on the hook for this debt because of a legal provision called the doctrine of necessaries, which, in many states, says that you are on the hook for the medical debts of your dead spouse. He was at his wit’s end until a reporter for the Wall Street Journal wrote a story that exposed what he’d been through, which eventually led to the remaining debt being forgiven by the hospital.
The best way to get your debt forgiven these days is to have the Wall Street Journal write about your case. But if you don’t have that, you’re up a creek. This example is egregious, but it’s not rare.
Sara Van Horn
What tactics have hospitals and debt collectors used to obfuscate their practices?
Luke Messac
Part of the reason debt collection has received relatively little treatment in the scholarly literature is that debt collectors cover up what they’re doing. If you go to their websites, there’s usually a tab that says, “For Hospitals,” where they’ll be very clear: we will pursue patients vigorously; we will get you your money. They’re clear about what they’re doing and how they’re doing it. But when they talk to the public, it’s never with that language.
In 2016, John Oliver did a segment on the Debt Buyers’ Association in which he went to their conference and uncovered their tactics, which seemed completely anathema to the spirit of health care. That same year, Human Rights Watch wrote a report about debt buying and interviewed folks in the Debt Buyers’ Association.
They were facing a lot of critical press, so the next year, they changed their name to the Receivables Management Association. The words “receivables management” and “revenue cycle management” (another term used by the industry) don’t mean much to most of us — they’re so anodyne — whereas with “debt collector,” you’ve got the vision of someone trying to break your kneecaps.
When debt collectors talk about their work, they talk about conferring “dignity” on debtors or about circulating money in the economy, as if it’s not just tearing dollars from the hands of poor patients. It’s important for them to not be clear about what they’re doing, but it doesn’t serve us if we want to know how the system works.
Cal Turner
Could you talk about your own story? How did you learn about this issue, and how did you get involved?
Luke Messac
In residency training, I had a number of experiences with patients who asked me how much their care would cost. I didn’t know the answer.
Patients would also show up too late: I had one woman who showed up with advanced cancer, with a large, painful mass that had been growing for months, and when I asked her why she’d waited so long, she said that she didn’t want to leave her family with unpayable debts. That fear of financial toxicity was so powerful that it led her to sit in agony at home until she finally came in and just wanted morphine.
I’d read that some hospitals were suing patients, but I didn’t think my own were doing it. I thought it was a rare, extraordinary practice that only the most unfeeling executives would ever sign up for. But then I went to my own courthouse to take a look and saw that my own hospitals were listed, time and again, as the plaintiffs, and the patients were the defendants in these lawsuits. I found out that my hospital was suing folks who were living on Social Security disability, recent immigrants, single moms — people who could not afford to pay their bills and were being expected to ruin their financial lives even further.
At that point, I wrote an article in a local blog that immediately got me in hot water with the hospital. I had a lot of meetings with executives to talk about what I’d written and how I was wrong because the hospital didn’t sue patients. Once the hospital, to its credit, started looking into this further and realized that its debt collection agency was still suing patients under the hospital’s name, it did stop the lawsuits.
Realizing how widespread this practice is changed my whole view of what medicine is in this country and how much harm we are doing to patients. Ignorance was no longer an excuse.
Sara Van Horn
Are there any collective efforts underway to eliminate medical debt collection?
Luke Messac
There are all sorts of proposals, from charity work to moderate reform to radical reimagining. There are state-level reform efforts to stop hospitals from putting so many patients in debt.
The nonprofit RIP Medical Debt is organizing students and churches to buy up people’s debts and forgive them. But that is a controversial practice, because you’re buying debt from a debt buyer or hospital that should be forgiving that debt. A lot of the folks who started that work, who grew out of Occupy Wall Street and now call themselves the Debt Collective, are working toward a world where medical debt does not exist by organizing unions of debtors.
There are other related efforts, too, including the many organizations advocating for Medicare for All, which would, if done right, make medical debt a thing of the past. They have been pushing for a single-payer health system in which patients are not charged at the point of care, but rather all health financing is done through progressive taxation.
Helping us imagine a world where we no longer have to talk about debt collection because there is no medical debt is ultimately the aim of this book. We’re not just talking about debt collection because it should be done more humanely. It shouldn’t be done at all. A world in which patients are made to pay for their care is inevitably a world where some people don’t get it.