We Need a Movement Against Vaccine Apartheid
Vaccine apartheid has built a giant variant factory that threatens us all — and it's caused by private ownership of pharmaceutical production and the indifference of Western governments. We need a movement demanding an end to it.

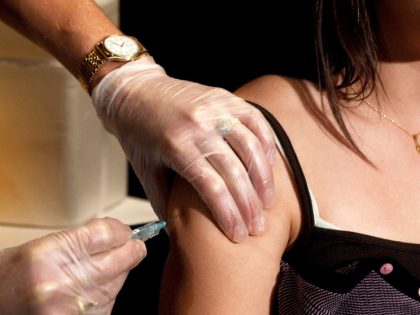
Army Specialist Angel Laureano holds a vial of the Pfizer / BioNTech COVID-19 vaccine. (Lisa Ferdinando / US Department of Defense)
It’s time for a revival of the anti-apartheid movement, crossed with Act Up — the heroic campaign in the ’80s and ’90s against HIV/AIDS injustice — but this time against global vaccine apartheid.
There is no other issue that comes close to being as important. It’s not just about justice, and still less about charity. It is a matter of self-interest, because no one is safe until everyone is safe. Vaccine apartheid has built a giant variant factory that threatens us all.
With vaccination rates across much of the West high (although far from high enough), regions are beginning to open up from a year and a half of lockdowns and other public health measures. While the Delta variant is driving up case counts in Britain, the United States, and a few other countries in the Global North, this time, such surges in cases are not being mirrored by surges in deaths, thanks to the vaccines.
Yet the situation is far bleaker elsewhere.
In the past week, Africa has recorded a 43 percent week-on-week rise in COVID-19 deaths. The continent’s case fatality rate (the proportion of deaths among confirmed cases) is now at 2.6 percent, compared to the global average of 2.2 percent. The situation for those admitted to intensive care is a grim toss of a coin: 48.2 percent die compared to a global mortality of 31.5 percent. The latest surge in cases, steeply rising for six weeks now, is a product of economic frustration at social distancing measures and other restrictions, the spread of the highly transmissible Delta variant of the virus, and abysmal access to vaccines.
The situation is compounded by poor health infrastructure with limited access to essential supplies and equipment, particularly oxygen. Countries are facing what Matshidiso Moeti, the World Health Organization’s (WHO) regional director for Africa, calls a “double barrier” of vaccine scarcity and treatment challenges.
Vaccine makers Pfizer, AstraZeneca, and Johnson & Johnson had, as of May, paid out $26 billion in dividends to shareholders, as well as share buybacks to goose stock prices over the last year, according to the People’s Vaccine alliance, a coalition of development and medical charities and NGOs. This same sum would be enough to vaccinate the whole of Africa. Another comparison from the same coalition is no less of an ethical grotesquerie: the pandemic has created nine new pharma billionaires, whose combined haul from the COVID-19 bonanza amounts to $19.3 billion — enough to fully vaccinate everyone in low-income nations 1.3 times.
While these least-developed countries are home to 10 percent of the world’s population, they had only received 0.2 percent of the global supply of vaccines, as of this spring. Eight existing billionaires with extensive COVID-19 vaccine pharma holdings saw their combined wealth soar by $32.2 billion since the start of the pandemic, enough to fully vaccinate the entire population of India.
Premature Third-Dose Bonanza
Meanwhile, though barely 1 percent of those in the least-developed nations have received even their first shot, the European Commission signed an agreement in June with Moderna for delivery of 150 million doses for third booster shots in 2022, and Israel, one of the fastest to vaccinate its population, this month started offering third doses to the immunocompromised.
The rationale is that we are confronted by a series of what the WHO calls “variants of concern.” These are mutations of the SARS-CoV-2 virus that not only allow it to spread more easily or that result in more severe illness, but that reduce vaccine effectiveness. The Beta, Delta, and Gamma variants of concern were first identified in countries with low vaccination rates: Brazil, India, and South Africa. The fourth variant of concern, Alpha, emerged in the UK, but in September last year, prior to high levels of vaccination. Epidemiological evidence is still being gathered to understand the exact threat posed by the Lambda variant “of interest,” but preliminary data suggest that it can infect cells more easily. It comes from Peru.
The reason is simple: unvaccinated people that get infected are variant factories. Most mutations offer no reproductive advantage or even actively harm reproduction. But occasionally, a mutation occurs that does offer an advantage that allows it to outcompete the other lineages of the virus and, over time, establish itself as the dominant one. These are the variants of concern. And the more people who are unvaccinated, the greater the chance of the emergence of such variants of concern. Conversely, the more people who are vaccinated — especially as it is now clear that the vaccines are not just extremely good at preventing symptomatic disease but also block most transmission — the fewer the variants of concern. A virus that cannot spread cannot mutate.
So far, the mRNA vaccines are holding up well against the variants of concern we have encountered. Other vaccine platforms are also performing decently, albeit less well. But researchers are warning that they worry about the next crop of variants, ones that really will be able to challenge the vaccines.
And at some point, if more variants emerge whose vaccine escape renders our existing suite of vaccines significantly less effective, then boosters may well be needed. But not yet.
After Pfizer requested another emergency use authorization, this time for a booster, the US Food and Drug Administration (FDA) and Centers for Disease Control and Prevention (CDC) issued a joint statement obliquely critiquing the firm for its booster boosterism. “Americans who have been fully vaccinated do not need a booster shot at this time,” they said, adding that they are “engaged in a science-based, rigorous process to consider whether or when a booster might be necessary.” While this process may consider data from pharma companies, it “does not rely on those data exclusively . . . We are prepared for booster doses if and when the science demonstrates that they are needed.”
Dr Tedros Adhanom Ghebreyesus, the director-general of the WHO, complained in a video last week about countries galloping toward third doses while the majority of the world suffocates and dies waiting for their first: “If there is one word that can explain it, it’s ‘greed.’”
Although it is understandable how the WHO chief might rage at what appears to be a moral compass broken beyond repair on the part of these pharma executives, his explanation is not actually correct.
It is not that the CEO or executives or shareholders of Pfizer, Moderna, and the rest are greedy. If this were true, to fix the problem, all we would need to do is find people who are not greedy to lead our pharmaceutical companies. The reality is that these firms have no choice but to delimit access, whether through patent protection or pricing structures or government lobbying or onerous demands on recipient countries in the developing world or reluctance to pay the costs of expansion or technology transfer.
If they do not engage in such behavior, they will be undercut by any competitor that does. Even if the most ethical human on the planet were appointed to head these companies, she would be forced by market incentives to do the same. (This is why firms that set out to be ethical, from Lush to Etsy to Google, so disappoint us when they end up “being evil” after all.)
Annual COVID Jabs for the “Endemic Market”
It is unlikely that we will actually come across any statements from CEOs so gauche as to admit that they must be hoping for ever more variants of concern, but privately, for them, Delta, Lambda, and their friends must be developments to be devoutly wished for.
This is because, if the pandemic ends, however much money has been made will be less than what would otherwise be made if it becomes a forever pandemic. Vaccines suffer from the same fatal flaw of under-profitability that has caused large pharmaceutical firms over the past four decades to abandon most antibiotic research and development: once an infection has cleared up, the patient doesn’t need to buy this commodity anymore.
Chronic conditions are much more profitable, because a patient must continue to take the drug (or whatever form of therapy) indefinitely, sometimes every day, for the rest of their lives. Vaccine research and development has suffered from a lack of interest on the part of large pharmaceutical firms for about as long, and for the same reason. But regular booster shots would turn the COVID vaccines from a once — or twice — and done affair into an annual or even biannual opportunity for profit.
The pharma executives are understandably being as delicate as possible in discussing the issue of variants of concern and consequences for profits. They do not want some journalist to catch them rubbing their hands with glee, but at the same time, they need to reassure investors of the likelihood of repeats of 2020’s and 2021’s spectacular revenues. During a first-quarter earnings call with shareholders, Pfizer CEO Albert Bourla reassured them that there will be a need for annual boosters “beyond ’22 and ’23.”
“This is the reason why basically all governments of the world are now discussing with us about procurement agreements for ’22, ’23 and ’24,” he added.
The firm’s chief scientific officer, Mikael Dolsten, added that “the inability to control [the virus] across the globe will, of course, lead to numerous changes in the viral mutation rate.” Rather than “hoping that herd immunity across the globe can be established,” the world will likely need to rely on regular boosting and other continued public health measures instead.
Moderna told investors a similar story during its own spring earnings call in response to worries from them that vaccination rates were slowing. CEO Stéphane Bancel was quick to reassure them. “We believe that, over the next six months, as the southern hemisphere enters its foreign winter, we could see more variants of concern emerge. We have said for right now that we believe booster shots will be needed, as we believe that the virus is not going away.”
As the firm pivots to what a Goldman Sachs investor called an “endemic market,” meaning one where the virus is permanently entrenched, the firm’s goal is now to have a seasonal flu vaccine combined with a COVID variant booster in a single-dose product that one receives every winter at the pharmacy or doctor’s office.

This is a crucial moment of honesty, at odds with what public officials continue to say about needing to reach high vaccination rates above 80 percent to achieve global herd immunity. The capitalists have given up on that as a goal. And while they are making it clear that they do not personally desire this situation, they are also making it clear to investors that it is good for the bottom line.
It is worth noting that, last year, during the height of Black Lives Matter protests, the heads of Pfizer, AstraZeneca, Johnson & Johnson, and over a dozen other pharmaceutical firms — including Merck chief Kenneth Frazier, Big Pharma’s only African American CEO — issued statements in support of the movement and committed to building more diverse workforces and boards. Pfizer and others even pulled ads from Facebook over concerns at the spread of racism on the platform. But there are 1.3 billion black and brown lives in Africa who one can be sure would much rather be vaccinated against this plague than read how much pharma executives learned about themselves at a Robin DiAngelo White Fragility workshop.
Yes, Patent Protection Really Is a Roadblock
There are those who will argue that “patents are not the problem” and that the barrier to more rapid production and distribution of COVID vaccines is instead the limited global production capacity, both of vaccines themselves and of the dozens of often-specialized inputs used to make them.
The Biden administration, alongside Russia and China, have thankfully rejected this position and endorsed the proposal first suggested by India and South Africa and since backed by more than one hundred other countries that provisions within the World Trade Organization’s Trade-Related Aspects of Intellectual Property Rights (TRIPS) Agreement for IP waivers during emergencies be invoked. But the EU, UK, Japan, South Korea, Australia, Canada, and other rich nations remain opposed (although, after weeks of wavering on the waiver, French president Emmanuel Macron now backs Joe Biden).
German chancellor Angela Merkel makes precisely this argument about the need for a focus on enhancing manufacturing capacity to defend her opposition to such a waiver. If that is not the priority, and we waste time on IP waivers, we will only undermine pharmaceutical innovation. Private companies need to be compensated for the risk they take in developing new drugs and other therapeutics, the argument goes.
The second part of her argument can be dismissed straightforwardly: in fact, most of the innovation for the suite of COVID vaccines was performed by university or government laboratories in the first place, and most of the bankrolling of development, clinical trials, and manufacturing was carried out by taxpayers.

But even the first aspect of the argument, which has some truth to it, nevertheless misses the point that even if patent protection is not the primary obstacle to adequate production of vaccines, it remains a major obstacle.
Vaccine licenses have been granted by the IP holders to only a relatively small handful of vaccine manufacturers restricted to those in richer countries and middle-income countries such as India. The pool of manufacturers that could be producing vaccine doses, particularly those using the more conventional vaccine platforms, is much larger than these licensees. As an editorial in the science journal Nature arguing against vaccine patent protections during the COVID emergency noted, “Unless manufacturing and supply can be distributed more evenly, researchers forecast that it will be at least another two years before a significant proportion of people in the lowest-income countries are vaccinated.”
It is true that the pool of manufacturers that could in principle be producing doses of mRNA vaccines is far smaller, perhaps close to nil. But there are ways to speed up and expand technology transfer to factories for this vaccine platform as well, and, crucially, the barrier to this is primarily the very same competition in the market that drives the need for aggressive patent protection.
We know this from what Moderna CEO Stéphane Bancel told investors when they asked if he was worried about Biden’s endorsement of an IP waiver. He said he isn’t losing a minute of sleep. “It doesn’t change anything for Moderna.”
Last October, the company said that it wouldn’t enforce its COVID-related patents during the pandemic. But this was no selfless act of charity on the part of Moderna. They won a slew of good PR for the announcement, while knowing it was meaningless so long as almost no one knew how to produce mRNA vaccines.
“There is no mRNA in manufacturing capacity in the world. This is a new technology. You cannot go hire people who know how to make the mRNA. Those people don’t exist. And then, even if all those things were available, whoever wants to do mRNA vaccines will have to buy the machines, invent the manufacturing process, invest in verification processes, analytical processes.”
This can, in principle, be overcome via technology transfer to multiple manufacturers. The term describes the transmission of proprietary knowledge about a product, its manufacturing processes, and the necessary analytical methods for quality assessment. It is a crucial step in all drug development, passing all know-how from the site of and brains behind the original innovation to a larger manufacturer.
But tech transfer isn’t easy or cheap. Novavax, whose protein-subunit-based vaccine platform is already used for multiple existing vaccines for the flu, hepatitis B, and HPV, should require a much more straightforward process of tech transfer than that needed for the completely new mRNA vaccines. The firm depends on a team of tech transfer specialists that have traveled around the world to train people. It takes many months to perform this task. And even here, with this much simpler tech transfer process requiring training related to largely existing technologies, Novavax is struggling to kick off production with a partner facility this year. The more manufacturing facilities that require such training, the more such tech transfer teams will be spread thin. Finally, if there is no financial benefit, and perhaps even a loss, resulting from hiring and setting up more such teams, why would a company do it? It is hard to set up more such teams to do the training, for that is itself a process of tech transfer. One cannot just snap their fingers and make tech transfer happen.
The WHO is aware of this very problem, which is why, in May 2020, they established the COVID-19 Technology Access Pool (C-TAP), initially at the prompting of Costa Rica, and subsequently the mRNA vaccine technology transfer hub, specific to this vaccine platform. These hubs aim to streamline the tech transfer process. Instead of training those at a facility one by one, these platforms were formed to provide a one-stop shop to link the developers of not just vaccines but all essential health technologies such as personal protective equipment (PPE), ventilators, and diagnostics and testing materials with experienced local manufacturers in developing countries. The C-TAP transfer process also, crucially, acts through public health–driven voluntary, nonexclusive, and transparent licenses.
But for this tech transfer streamlining process to work, the owners of the IP have to be willing to participate. And so far, C-TAP has failed at its goal, due to the widespread refusal of these firms to participate. The rationale is the same as the resistance to waiving patents: a greater diffusion of vaccine know-how undermines their monopoly no less than a TRIPS waiver does.
Vaccine Input Bottlenecks
These firms are not the only ones at fault. The cost of not just tech transfer but also, even more important, scaling up regional manufacturing capacity and production of the inputs for vaccines will be immense. As already shown, the profits gained by the vaccine producers would be sufficient to pay for this, but then this throws into question the rationality of private for-profit pharmaceutical production. In the long term, society must consider whether pharmaceutical production should be taken into the public sector in toto, using the postal service model, wherein profitable drugs, vaccines, and other therapeutics cross-subsidize production of unprofitable ones. This is admittedly a big ask, and we do not have time in the current emergency to engage in such a nationalization endeavor.
We need, in the meantime, to push Western states to do four things. First, they must spend whatever it takes to scale up globally distributed vaccine and vaccine input production. The tens of billions of dollars this will cost is dwarfed by the trillions being lost as a result of our inability to wrestle this pandemic to the ground. Pure capitalist rationality requires such state intervention to correct this market failure long before we approach concerns of health justice.
Second, there must be a replication of the state direction of private investment via aggressive application of the Korean War–era Defense Production Act (DPA) that occurred under the Trump administration and then was sharply expanded under Biden, to shepherd production and distribution of PPE, ventilators, other key pieces of medical equipment, and the vaccines themselves — as well as their material inputs — on the basis of epidemiological rationality rather than the amoral profit-driven anarchy of the market. There are some nine thousand different, often highly specialized inputs required in vaccine manufacturing, sourced from three hundred different manufacturers in thirty different countries, according to an assessment by the International Federation of Pharmaceutical Manufacturers and Associations (although not every individual vaccine requires all these inputs). Production of these inputs is also concentrated primarily in the United States and Europe. One bottleneck already occurring in India comes from insufficient supply of plastic bioreactor bags. Another is a lack of filters for purification and sterilization. There are many other examples, from glass vials and stoppers, to especially critical inputs such as adjuvants (which enhance the ability of the immune system to mount a response), lipid particles, nucleic acids, amino acid phenols, acyclic amides, lecithins, and sterols.
One of the reasons government needs to both supervise supply chains and be the funder of first resort is that, once the emergency is over, such radical expansion of manufacturing capacity may sit idle, at least until the next pandemic. Here again, private pharmaceutical firms and the firms that produce their inputs have no interest in investing in idle capacity.
It is true that one of the reasons places like India face input shortages has been the use of the Defense Production Act (DPA) to prioritize input production for American vaccines and other medical supplies. However, this fact should not be wielded to undermine the concept of economic planning of production, but rather to argue that economic planning should be enacted in the interest of all, and not just Americans (and, in any case, the faster the rest of the world is safe from COVID, the faster Americans will be, too).
The DPA was deployed to overcome domestic market irrationality of production and distribution, but with indifference to irrationality of production and distribution beyond US shores. This time, DPA coordination of supply chains must be in the service of international and not just domestic vaccine production. Across the Atlantic, much of the same must occur. The EU may not be a state and has no equivalent to the DPA, but the largest member states have no such institutional obstacles.
Third, states must follow the Biden administration’s lead and accept a patent waiver during the emergency. Fourth, all relevant states must compel holders of IP to participate in the WHO’s technology transfer platforms, C-TAP and the mRNA transfer hub, free of intellectual property constraints.
And at some point, a conversation needs to start about a global, public anti-pandemic service that maintains sufficient industrial capacity for vaccines, inputs, and other aspects of pandemic response independent of the need for profit. Like the fire service, it is something we all pay for through our taxes to be there whenever it is needed.

In June, some twenty-five prime ministers and presidents, including the leaders of France, Germany, the UK, and Spain, issued a call for a “pandemic treaty” to build a new, more robust global health infrastructure for future pandemic preparedness and response. This is to be welcomed, but we should remember that many of those calling for such an architecture are the same ones that undermine today’s pandemic response in the name of profit. We have to develop our own independent conception of what a just global pandemic infrastructure would look like.
And because any future pandemic infrastructure necessarily requires sufficient authority and funding to coordinate medical materiel production and allocation, this entity, a super-WHO, would supervene over elected governments. If that entity itself is not democratically accountable, it will not have the mandate to override such governments. The European Union, the World Health Organization, the International Monetary Fund, and the World Bank are all examples of supranational entities with incomplete or no democratic legitimacy. Without a popular mandate, their degrees of freedom of maneuver are limited from the outset. Thus, discussion of some sort of architecture of global democracy is now unavoidable in the medium term, even if, for the time being, the focus must be on the immediate emergency.
A Global Sharpeville Massacre
On March 21, 1960, police in the South African township of Sharpeville fired on a crowd of seven thousand who were protesting against internal passports used to segregate the population, killing or wounding some 250 people, including women and children. The atrocity was a catalyst internationally for the founding of the anti-apartheid movement, and domestically for the shift of the African National Congress from civil disobedience to armed resistance.
Today, we confront a new, global, but slow-moving Sharpeville, a scandalous inequality of access to life-saving vaccines that not only condemns to death millions in the developing world for the sake of profit but threatens every one of us in the developed world, too.
Let today’s scandal catalyze us as well, to create a new anti-apartheid movement, but this time against vaccine apartheid.
A coalition of NGOs and charities such as Amnesty International, Oxfam, Global Justice Now, and Public Citizen have come together to form the aforementioned People’s Vaccine campaign, backed by a raft of former and current prime ministers and presidents. This effort is crucial: these groups have the funds and connections to mount an effective “inside strategy” of lobbying and communications efforts in the corridors of power in multiple countries, as well as bankrolling critical, evidence-based research and analysis of needed next steps.
But there must be an “outside strategy” as well. The respectability of these NGOs, as necessary as it may be to ensure access to the halls of power, also curtails to some extent their ability to critique and suggest alternatives to markets. That’s fine as far as it goes, otherwise such access would be cut off. More important, while they can recommend and hobnob and schmooze, hoping that they can convince decision-makers of the need for change, they do not have the political leverage to force change. For this, there needs to be a demonstration to elites, both corporate and political, that vaccine business as usual will come at some considerable political cost.
Earlier this month, the New York chapter of Act Up, the militant HIV/AIDS campaign group whose direct-action stunts and die-ins during the height of the AIDS pandemic in the ’80s and ’90s were instrumental in forcing more aggressive governmental and corporate action to defeat that disease, blocked the street outside Pfizer headquarters, risking arrest, but this time in the struggle against COVID vaccine apartheid. Activists with People’s Action, Health GAP, and Justice Is Global, among other groups, dumped a series of body bags outside the White House alongside an Angela Merkel effigy during the German chancellor’s meeting with the US president. When Merkel visited Johns Hopkins University in Baltimore, Maryland, to receive an honorary degree in commemoration of her “principled global leadership,” a troop of students and alumni from the institution, home to one of the most prestigious medical schools in the nation, likewise mounted a flash protest against her.
Hopefully, these so-far small but important demonstrations are the opening guns of a much wider global protest movement against vaccine apartheid on the scale of the original anti-apartheid movement. Everywhere, the leaders of Germany, the EU, Britain, Switzerland, Japan, and Australia — the primary opponents to patent waivers — must be confronted with body bag dumps, protests, and similar actions. But, like that earlier movement, we must keep front of mind the central importance of basing such action among those with much more power to effect change than any number of marches or road blockades: workers, and in this case health care workers, who are able to withdraw their labor and challenge profits directly.
Multiple times during COVID, nurses, doctors, and other health care providers have gone on strike. In February 2020, Hong Kong health care workers struck, demanding border closures and access to PPE. In June, their Zimbabwean counterparts struck again over lack of access to PPE and low salaries. In August, South Korean doctors mounted a nationwide strike. In November, it was Pennsylvania nurses’ turn to strike, following protests in Washington, New York, and California. In May this year, burnt out by COVID, French intensive care nurses struck for better pay. Health care workers in Bosnia, Kenya, Peru, and Spain also number among those who have taken industrial action over some aspect of the pandemic. All have included demands related to inadequate responses to COVID, in particular insufficient protection for frontline workers.
Today, we can read about how such workers are livid at the surges they are once again having to confront. One COVID ward consultant, writing anonymously in the Guardian, speaks of their barely containable fury at those who have refused to be vaccinated, in particular for the threat they pose to those with compromised immune systems for whom the vaccines do not work as well. This anger is entirely legitimate, but the threat to their hospitals and to the rest of us caused by the inability of billions in the developing world to access vaccines is greater still. Let’s channel that righteous rage of health care workers thinking they can do little more than write letters full of resignation and despair into strikes against vaccine apartheid that can force governments to take the necessary action.
Health care workers and ethicists have long debated whether it is morally acceptable for the former to go on strike. The conclusion in general is that it is ethical if greater harm is likely should they decline to do so. In addition, a range of measures are taken to ensure they cause no harm to patients, such as limitation of disruption of health care delivery to cancellations of outpatient appointments and elective surgeries. Refusal of non-emergency service to elected representatives until they commit to ending vaccine apartheid might be another tactic that targets those responsible for the atrocity while avoiding antagonizing those members of the public who are not. Another action on the labor wish list might be for pharmaceutical firm employees, warehouse staff, and drivers to find creative ways to undermine profits elsewhere for these companies while ensuring COVID vaccines are still distributed.
But such specifics of strike strategy are less important at this point than the simple recognition that protests, occupations, civil disobedience, and direct action, as urgent these are — especially if coordinated across national borders — will be immeasurably strengthened if they are joined by industrial action taken by health care workers on the COVID front lines and by pharmaceutical firm employees.
For those of us outside the major cities where the headquarters of the Pfizers and Modernas of the world are based and government leaders craft laws, there are hundreds of other actions we can take as well, from raising awareness and smaller-scale protests to connecting with local health care workers in the hope that industrial action spreads as widely as possible.
So, let’s get on it. This week, get out there and start up or join an “End Vaccine Apartheid” campaign group or action wherever you are. Please forgive this double-vaccinated Westerner for borrowing the great slogan of the original anti-apartheid struggle, but we need to raise it once more: Amandla Ngawethu! Power, it is ours!